By Anna Vlugt, Editor-in-Chief
Introduction:
Approximately 172,000 organ transplants are performed every year (Mendoza, 2025). However, anywhere between five and 10 percent of these life-saving surgeries involve illicit practices: the organs come from the black market (United Nations Office on Drugs and Crime, n.d.). The following article attempts to address this problem by starting at its root and explaining the process from the ground up.
Beginning with a medical angle and a historical breakdown, the article will tackle the questions of why and how this trade exists while also briefly providing potential solutions which are being discussed by medical, legal, and security professionals.
Background: What is an organ transplant?
The term itself is defined as: an organ transplant is the removal and insertion of an organ into one’s body. However, there is much more to the procedure. First off, there are multiple types of organ transplants.
- “Autograft: Autotransplantation is the transplantation of organs and tissues from one part of the body to another in the same individual. Tissue transplanted by such “autologous” procedure is referred to as an autograft or autotransplant.
- Allograft: An allograft is a transplant of an organ or tissue between two genetically non-identical members of the same species. Most human tissue and organ transplants are allografts.
- Xenograft: A transplant of organs or tissue from one species to another. An example is porcine heart valve transplant, which is quite common and successful,” (Al-Bar, 2015).
This article will focus on the allograft.
Such surgeries have existed in theory since 700 B.C. However, they only began to occur in practice in the 1500s. The first successful transplant recorded in history was of a cornea, performed in 1905 in Czechia (Al-Bar, 2015). Since then, kidneys have become the most commonly transplanted organ, followed by the liver (see figure 1) (ACAMS Today, 2021). Other ‘common’ transplants include the heart, lungs, and intestines (U.S. Department of Health and Human Services, 2024).
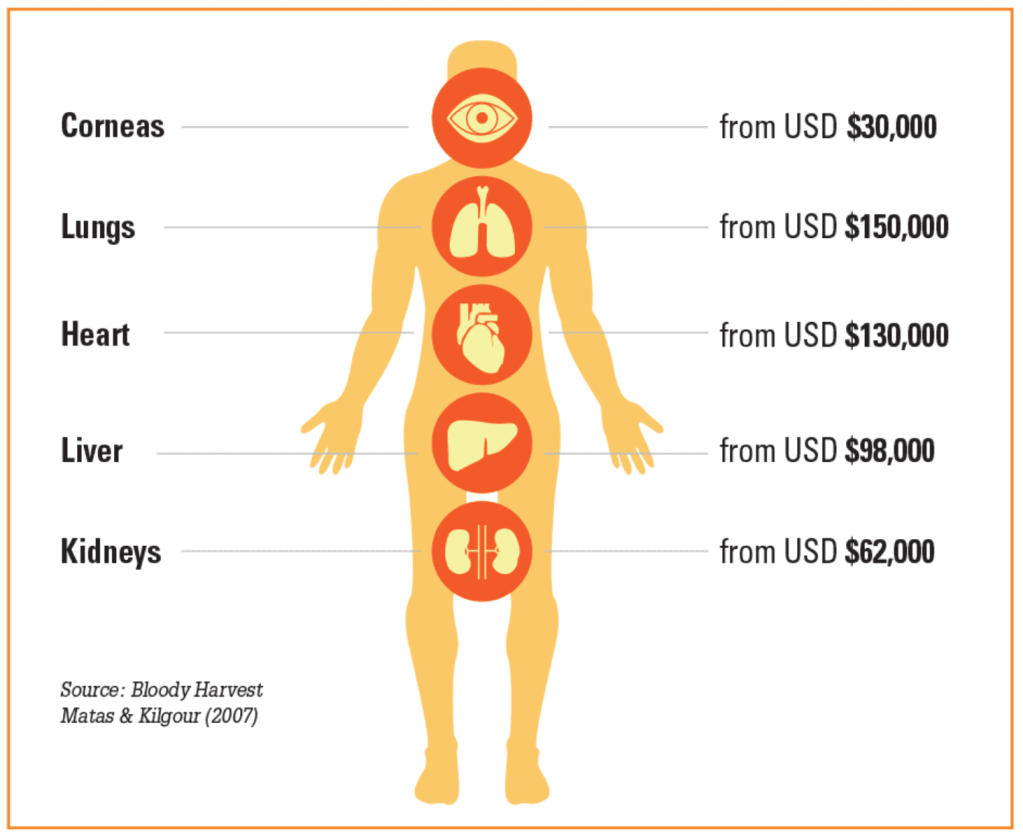
Figure 1 (ACAMS Today, 2021)
Scarcity of Organs:
Despite the development of the procedure itself, there are still many boundaries to organ transplants. The primary reason for this is due to supply being significantly lower than demand.
This ‘lack’ of available organs can be attributed to several causes, one of which is people not consenting to becoming donors. In the Netherlands, non-consent nearly doubled between 2020 and 2024, whereas consent only increased by ⅓ (see graph one). In this specific case, the increase in both categories is likely attributed to the Netherlands introducing “The Donor Act,” which stated all residents over 18 must submit a preference, or else they would be recorded as having “no objection to donation” (Statistics Netherlands, 2024).
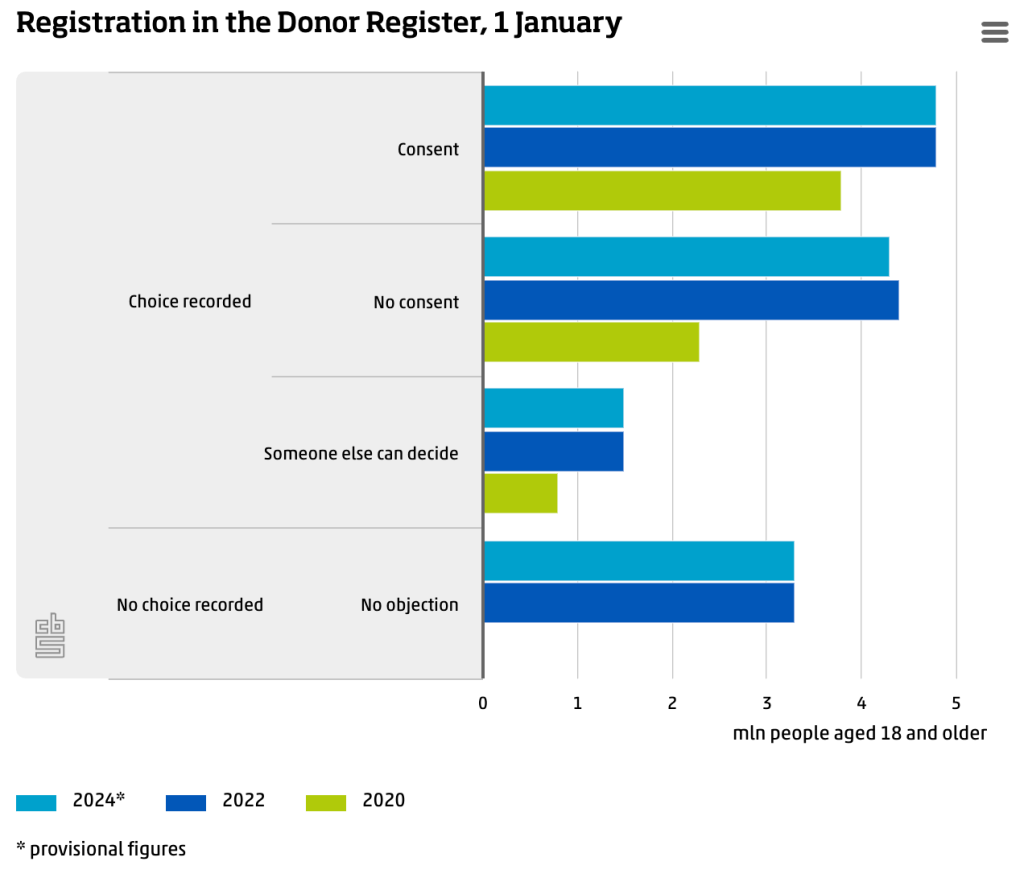
Graph 1 (Statistics Netherlands, 2024)
Given the sheer amount of people who are unwilling to donate their organs, the question of why must be addressed. Although there is no one reason, and it is impossible to identify all potential reasons, some are more common than others. A communication study (see table one) conducted by four university professors in the United States (U.S.) revealed that a fear of premature declarations of death, mistrust in doctors, and a fear of mistakes were the most common reasons for non-consent. The participants came in pairs, resulting in 78 total dyads, 60 of which cited the aforementioned reason(s) (Statistics Netherlands, 2024).
Religious beliefs were mentioned by the dyads most often, however only seven of them viewed their beliefs as a reason to not donate, showing a discrepancy between reasons the participants could identify versus those that they actually identified with (Morgan et al., 2008).
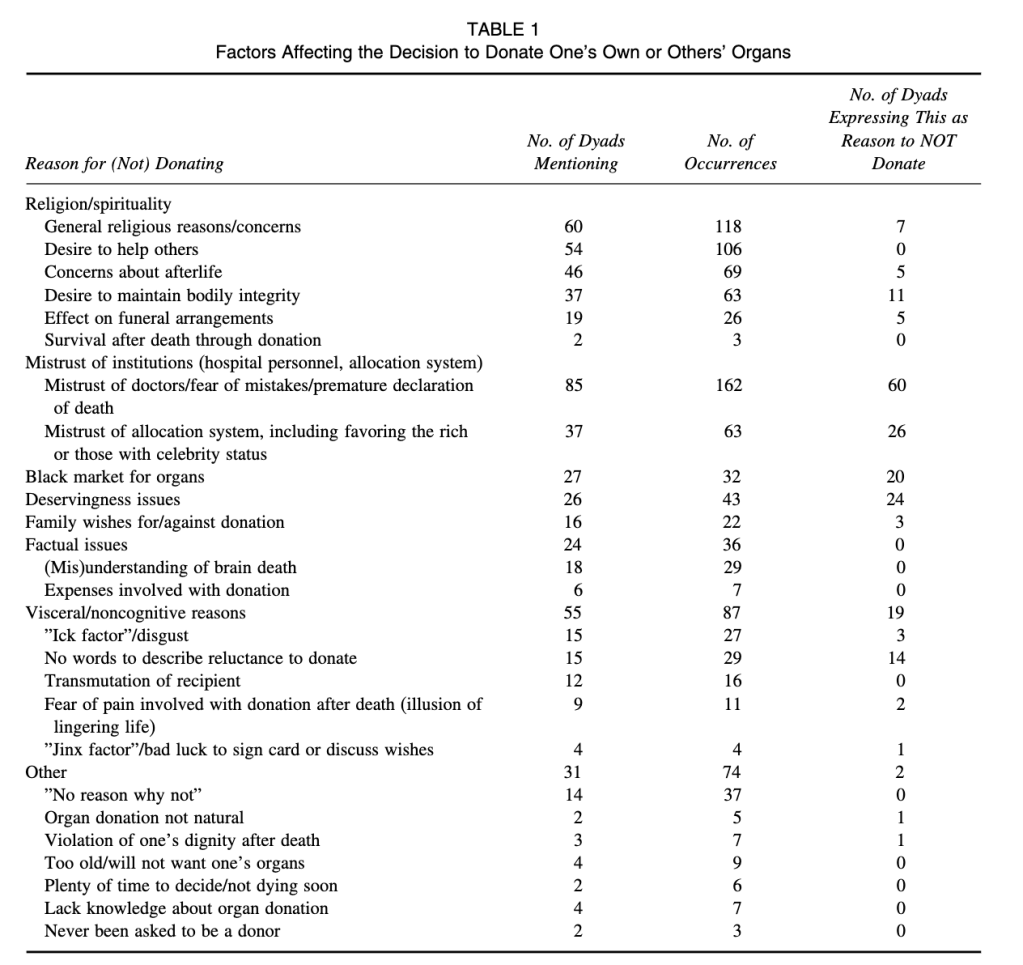
Table 1 (Morgan et al., 2008).
The lack of donors is a major contributor to organ scarcity; however, it is not the only factor. In many cases, the organs of someone who has consented to donation are not able to be used in a transplant. This can be attributed to a litany of reasons, most of which relate to the condition of the organs in question.
Although organs are desperately needed, several conditions must be met before the donation can occur. Assuming the deceased has already consented to being a donor, it is also of extreme importance that they pass in a hospital. If the donor dies at home or another location, they become unable to donate as their organs begin shutting down (almost) immediately, starting with the heart and eventually all other vital, transplantable organs. Upon shutting down, organs are no longer able to be transplanted, no matter the donor status (Cleveland Clinic, 2025).
However, if a person in the hospital passes away and is deemed brain dead, then it is possible to use their organs for transplant, assuming other conditions are met. Further, some illnesses or diseases may automatically rule one out as an organ donor. For example, a person with Ebola or HIV (with the exception of if it is transplanted to someone else who is HIV-positive) cannot be an organ donor, even if the cause of death is unrelated (NHS Blood and Transplant, n.d.).
The condition of one’s organs must be taken into consideration before they are transplanted. Although someone who drinks alcohol can donate their organs, some organs may not be suitable for transplant if the deceased abused alcohol, e.g., the liver (NHS Blood and Transplant, n.d.).
Because all organs must meet these (and several other) conditions, the amount of usable organs is significantly less than the amount of people who need them, resulting in approximately 13 people (in the U.S) dying while waiting for an available organ every day (Health Resources and Service Administration, 2025). This scarcity is what leads to the underground/illegal organ trade.
Organ Trafficking:
Despite the known illegality of buying and selling human organs around the world (with the exception of Iran), the crime still occurs on a semi-regular basis, with the start-point being primarily in the Global South (Columb, 2024). North and West Africa have been identified as a particularly vulnerable region due to much of the population being impoverished or displaced (INTERPOL, 2021). Several other countries are considered organ trafficking ‘hotspots’ with the trade including countries starting in Eastern Europe, to the Middle East, and going as far as China and the Philippines (Columb, 2024). These specific countries are likely considered ‘hotspots’ as many of them have economic or political instability, making their population more vulnerable and desperate.
Generally speaking, victims of organ trafficking are already vulnerable and are offered money in return. Whether it is due to their economic, educational, or immigration status, giving an organ can be seen as a ‘way out’. This strategy, however, rarely succeeds, resulting in donors not being given (all of) the money they were promised and often receiving limited to no post-operation care.
The most common organ trafficking scenario involves a broker coercing someone who falls into one of the aforementioned categories into giving up an organ in return for a ‘life-changing’ payment. This often turns into a pyramid scheme with those who were trafficked telling others about the ‘opportunity’ to make money, which almost never comes (Stumpf & Carney, 2024). Given the fragile status of the sellers, they are especially unable to ensure they are paid what is due. By committing the crime of organ selling and having other struggles (i.e., undocumented immigrants, criminals, etc.), the donors/sellers cannot report the crime, as it would result in their arrest as well (Columb, 2024).
Another scenario, albeit less common, involves people having their organs taken unknowingly or unwillingly. The United Kingdom faced a case of the sort in 2023 when a young man from Nigeria arrived for a job opportunity. It was later revealed that there was no job and that the man had been tricked into coming so his organ(s) could be harvested. The operation, luckily, did not occur, but the young man was still at risk due to the traffickers´ threatening to send him back to Nigeria (Lobel et al., 2023).
Ultimately, the underground organ transplanting ring involves a significant amount of manipulation of vulnerable people. This, however, is only the first part of the process. Once a person is found who is willing to sell their organ, the broker is ‘responsible’ for getting the organ to the operating table for the buyer.
Post-purchase:
Upon the collection of the organ as outlined in the previous section, the broker (who is occasionally the surgeon themselves) begins to involve other parties, one of whom being ‘the driver’ who is physically responsible for getting the organ from the country of origin to the country in which the recipient will have the operation (European Parliament, 2015) (the country in which the surgery is done is often not the same country that the receiver is from/currently resides in (Stumpf & Carney, 2024)).
Once this part of the process is complete (see figure 2) and the organ arrives at its final destination, the surgical procedure can begin. The form in which these surgeries are performed, or the doctors are involved in the crime, differs on a case-by-case basis (three common scenarios exist). For some transplants, the surgeon is already an existing part of the trafficking network (possibly an organizer/coordinator) and therefore, is aware of the organ’s history and that they are committing a serious crime. This often comes with a significant amount of money (European Parliament, 2015, p. 21). Alternatively, the surgeon is working at a legitimate hospital and is outside of the network. These surgeons are also aware that the transplant is illegal but choose to perform the surgery for the check that comes with it (Stumpf & Carney, 2024). The final (common) scenario involves a surgeon working at a legitimate hospital who is unaware of the situation or their participation in the crime. Subsequently, they do not receive additional payment, only their normal salary (European Parliament, 2015, p. 21).
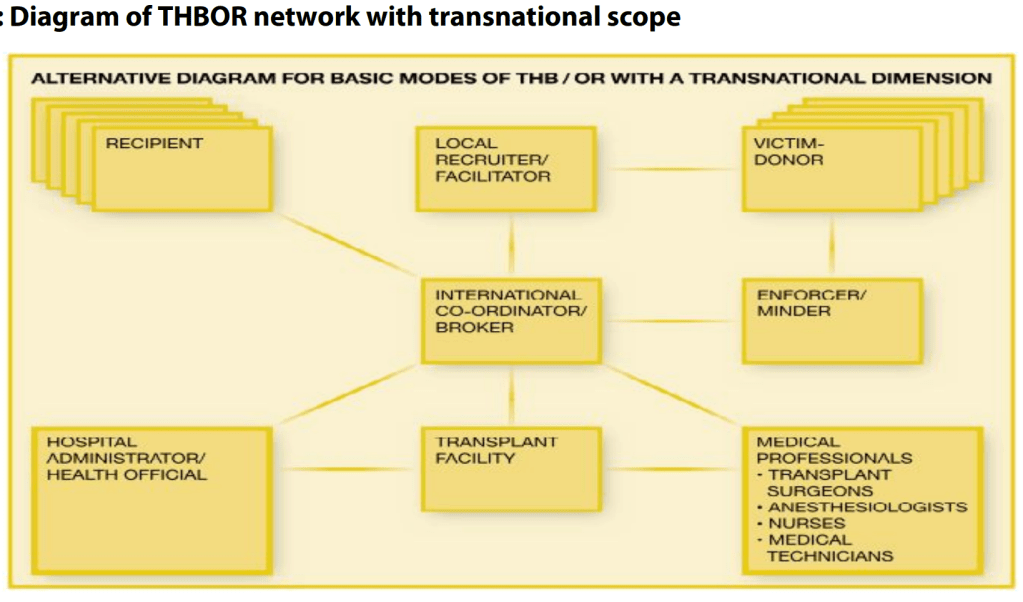
Figure 2 (European Parliament, 2015).
Post-operation Ethics:
Transplants of any kind are not simple surgeries and require a significant amount of post-operation care for the patient/receiver. As previously mentioned, most underground organ transplants are performed in countries where the receiver is not from or currently residing, resulting in the post-operation care needing to be done in their home country (or place of residence).
Once the transplant recipient returns home and visits their own doctor for post-operation care, it often becomes apparent that the patient received an organ illegally (Stumpf & Carney, 2024). This presents an immediate ethical conundrum for the doctor. By providing care to a patient who received an organ illegally, the doctor becomes involved in the original crime. However, not assisting their patient after the transplant directly violates the Hippocratic Oath.
The Hippocratic Oath is taken by medical professionals and consists of a few key points: non-maleficence and beneficence are the most relevant in this case. The former is more commonly known as the principle of “do no harm” and the latter relates to doctors acting in their patients’ best interest. By not providing medical care to their patient, the doctor is not acting in their patient’s best interest and may ultimately cause harm (Aikens, 2024). However, if they do provide care, they become complicit to the crime (Stumpf & Carney, 2024).
This situation forces doctors to choose between breaking their oath or the law, both of which have the potential to cause the doctor to lose their medical license.
Combatants:
Although there will always be people willing to break the law and participate in organ trafficking, certain actions have been taken to prevent and deter trafficking. The Council of Europe created an international treaty, the Santiago de Compostela Convention (Council of Europe, 2015), which went into force in 2018. Despite being of European origin, the convention is open to all countries. That being said, only 15 countries have both signed and ratified.
The goals of the Convention are specifically stated as follows:
“The purposes of this Convention are:
- to prevent and combat the trafficking in human organs by providing for the criminalisation of certain acts;
- to protect the rights of victims of the offences established in accordance with this Convention;
- to facilitate co-operation at national and international levels on action against the trafficking in human organs,” (Council of Europe, 2016).
The convention goes further to outline specific scenarios in organ trafficking, their consequences, and protection measures for victims.
In addition to the Santiago de Compostela Convention, the United Nations Convention against Transnational Organized Crime also specifically addresses organ trafficking (Duguay et al., n.d.). This ratified version of the convention predates the Santiago de Compostela Convention and serves as the first legally binding document that addresses trafficking with a universally agreed-upon definition. This document was further expanded upon and ratified by the Canadian government.
Moving across the Atlantic, Istanbul’s Declaration on Organ Trafficking and Transplant Tourism was a landmark declaration as it went further into detail on what organ trafficking is and the different variations. Further, Istanbul’s Declaration holds several purposes, including prevention and prohibition, as well as stressing the importance of legal and safe transplants (Duguay et al., n.d.).
The final piece of legislation worth mentioning is the United Kingdom’s (U.K.) Human Tissue Act of 2004. Although this is not specifically written for combating organ trafficking, it is meant to ensure that living donors have agreed to donate of their own volition. Subsequently, this helps to minimize the trafficking of organs within the UK (Duguay et al., n.d.).
Non-binding/non-legal combatants also exist. For example, the World Health Organization (WHO) has published several articles regarding organ trafficking (World Health Organization, n.d.). Despite these having little to no ‘impact’ on the trade itself, the WHO providing a significant amount of guidance may influence other countries that have legal authority to take further action.
Conclusion and Recommendations:
Although there are several laws and conventions to fight the underground organ trade, the problem still remains widespread and fuels a significant number of transplants. In addition to the legal efforts, alternative options for an organ trade are being researched. For example, some believe there may be ways to create an ethical organ trade (Pepper & Carrick, 2024). Even if a legal alternative were to come to fruition, there is still the risk of illegal operations.
As most of the previously mentioned legal documents mention, the protection of victims is of the utmost importance. Instead of attempting to solve this problem from the top down, a more effective alternative may be to help the victims first. By viewing illegal organ transplantation as a humanitarian issue, there may be a more effective way to reach a solution. If more effort went into helping those in vulnerable positions, those who believe donating an organ is the ‘only option’, the pool of victims will dry up, and slowly, the trade will become less fruitful.
Sources:
ACAMS Today. (2021, November 18). Organ trafficking: The unseen form of human trafficking. Human Trafficking Search. https://humantraffickingsearch.org/resource/organ-trafficking-the-unseen-form-of-human-trafficking/
Aikens, C. D. (2024, October 31). “do no harm” and medical malpractice. Carla Aikens Attorneys at Law. https://www.aikenslawfirm.com/do-no-harm-and-medical-malpractice/#:~:text=Key%20Principles%20of%20the%20Hippocratic,is%20absolutely%20necessary%20for%20treatment
Al-Bar, M. A. (2015, May 28). Organ transplantation. Contemporary Bioethics: Islamic Perspective [Internet]. https://www.ncbi.nlm.nih.gov/books/NBK500177/#:~:text=Types%20of%20Transplant,is%20quite%20common%20and%20successful
Cleveland Clinic medical. (2025, December 19). Death: What happens when you die. Cleveland Clinic. https://my.clevelandclinic.org/health/articles/23144-what-happens-when-you-die
Columb, S. (2024, September 10). “For me, there was no other choice”: Inside the global illegal organ trade. The Guardian. https://www.theguardian.com/news/article/2024/sep/10/for-me-there-was-no-other-choice-inside-the-global-organ-trade#:~:text=It%20is%20illegal%20to%20buy,at%20greater%20risk%20of%20exploitation%E2%80%9D
Duguay, J.-P., Hermon, B., & Smith, A. (n.d.). Trafficking in Human Organs: An Overview. https://lop.parl.ca/sites/PublicWebsite/default/en_CA/ResearchPublications/202083E#a4
European Parliament. (2015). Trafficking in human organs. European Parliament. https://www.europarl.europa.eu/RegData/etudes/STUD/2015/549055/EXPO_STU(2015)549055_EN.pdf
Explainer: Understanding human trafficking for organ removal. United Nations : Office on Drugs and Crime. (n.d.). https://www.unodc.org/unodc/en/frontpage/2024/June/explainer_-understanding-human-trafficking-for-organ-removal.html
Éditions du Conseil de l’Europe, Council of Europe Convention against Trafficking in Human Organs: Cets n° 216 and explanatory report: Santiago de Compostela (Spain) 25.III.2015 2 (2016). Strasbourg.
Health Resources and Service Administration . (2025, May). Organ Donation Statistics. Health Resources and Service Administration . https://www.organdonor.gov/learn/organ-donation-statistics
INTERPOL. (2021, September 30). North and West Africa: Interpol report highlights human trafficking for organ removal. INTERPOL. https://www.interpol.int/en/News-and-Events/News/2021/North-and-West-Africa-INTERPOL-report-highlights-human-trafficking-for-organ-removal
Lobel, M., West, K., & Stewart-Smith, M. (2023, June 27). Organ harvesting: Trafficked for his kidney and now forced into hiding. BBC News. https://www.bbc.com/news/65960515
Mendoza, J. (2025, December 17). Topic: Organ donations and Transplants. Statista. https://www.statista.com/topics/2389/organ-donations-and-transplants/#:~:text=In%202023%2C%20there%20were%20over,organ%20donations%20around%20the%20world
Morgan, S. E., Harrison, T. R., Afifi, W. A., Long, S. D., & Stephenson, M. T. (2008). In their own words: The reasons why people will (not) sign an organ donor card. Health Communication, 23(1), 23–33. https://doi.org/10.1080/10410230701805158
NHS Blood and Transplant. (n.d.). Who can become an organ donor?. NHS Blood and Transplant. https://www.organdonation.nhs.uk/about-organ-donation/who-can-donate/
Pepper, F., & Carrick, D. (2024, August 8). Illegal organ trafficking is big business, and vulnerable people are at risk. Could an ethical organ trade solve this?. ABC News. https://www.abc.net.au/news/2024-08-09/illegal-organ-trafficking-how-to-solve-it/104188548
Statistics Netherlands. (2024, August 28). Over 4 million people withhold consent for organ donation. https://www.cbs.nl/en-gb/news/2024/35/over-4-million-people-withhold-consent-for-organ-donation
Stumpf, A., & Carney, S. (Hosts). (2024, October 9). The underworld of organ trafficking [Audio podcast episode]. In Change Agents with Andy Stumpf.
Trafficking in human organs – frequently asked questions – countering the trafficking in human organs – http://www.coe.int. Council of Europe. (2015). https://www.coe.int/en/web/trafficking-human-organs/frequently-asked-questions
U.S. Department of Health and Human Services. (2024, June 17). Organ donation: Pass it on. National Institutes of Health. https://newsinhealth.nih.gov/2011/03/organ-donation-pass-it#:~:text=The%20kidney%20is%20the%20most,friends%20of%20the%20transplant%20recipient
World Health Organization. (n.d.). Transplantation. World Health Organization. https://www.who.int/health-topics/transplantation#tab=tab_1
Disclaimer of Liability:
While we are transparent about all sources used in this article and double-checked all the given information, we make no claims about its completeness, accuracy or reliability. If you notice a mistake or misleading phrasing, please contact centuria-sa@hhs.nl .
This article also contains links to other third-party websites, which have only been placed for the convenience of the reader and does not imply endorsement of contents of said third-party websites.


Leave a comment